Black Maternal Health in North Carolina
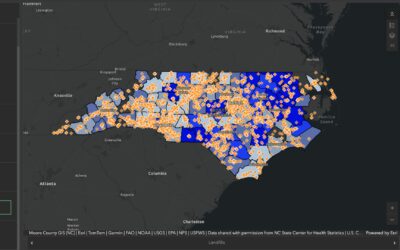
Black maternal health in North Carolina reflects persistent gaps in access, quality of care, and workforce representation. In many rural eastern counties, families face hospital closures, provider shortages, and transportation barriers that limit consistent prenatal and postpartum care. Maternal health outcomes are shaped not only by clinical services, but also by trust, cultural responsiveness, and sustained support beyond delivery.
Policy changes such as Medicaid expansion increase coverage, but coverage alone does not eliminate disparities. Addressing the Black maternal health crisis requires long-term investment in access, accountability, and community-based solutions.
Lactation Ambassador Program
We advance this work through our Lactation Ambassador Program, which focuses on workforce development rather than direct service. The program expands the pipeline of trained lactation professionals in Eastern North Carolina, equipping women, particularly women of color, with evidence-based breastfeeding education and community outreach skills.
By strengthening local capacity, we help ensure that Black mothers can access breastfeeding support from professionals who reflect their lived experiences and cultural context. This approach builds trust, improves postpartum support, and strengthens maternal and infant health outcomes over time.
Quick Points
- The Black maternal health crisis is an access to healthcare issue. Access to quality maternity care is a critical component of overall maternal health and helps to produce positive birth outcomes.
- Black women are 3 to 4 times more likely to die during childbirth. Black infants are 2.4 times more likely to die in the first year.
- 60 percent of pregnancy-related deaths are preventable.
- In Medicaid expansion states, the uninsured rate is nearly half the rate in non-expansion states.
- Rural areas in northeast and southeast North Carolina have low access to maternity care or live in a maternity care desert where obstetric care is unavailable.
Resources